MBSC - Weigh the Odds
Validated in clinical trials · Supported by multiple studies
App Summary
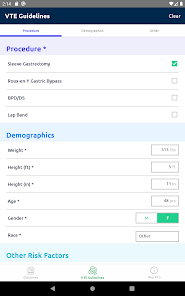
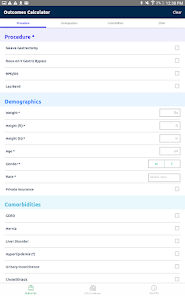
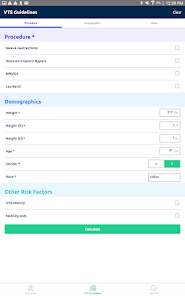
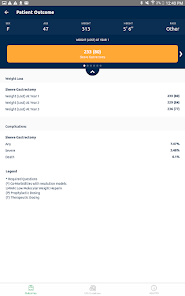
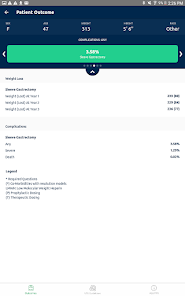
App Screenshots






Detailed Description
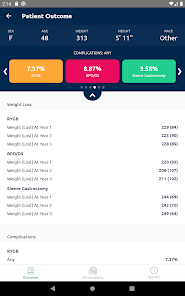
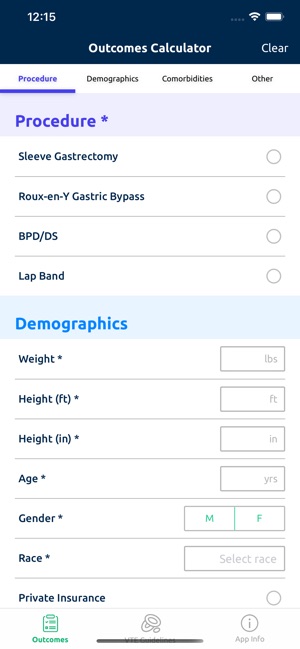
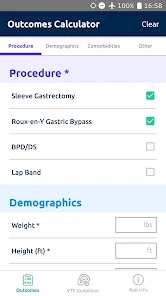
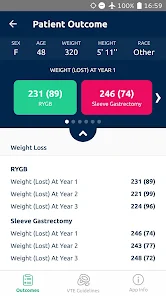
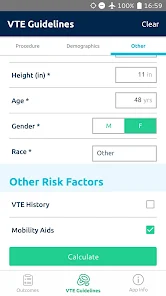
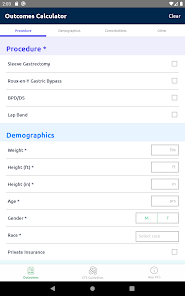
Functionality & Mechanism
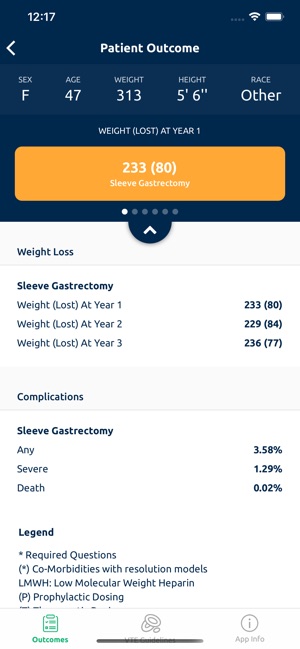
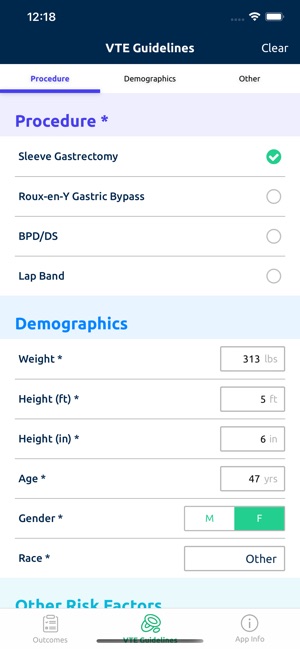
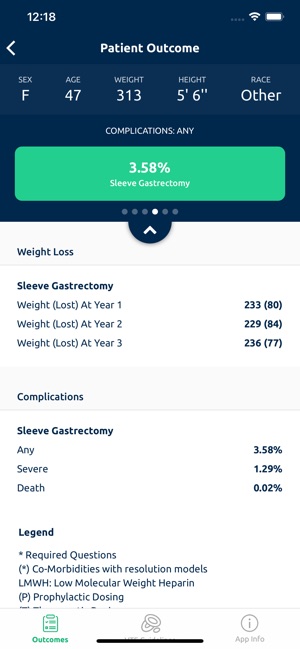
Developed by the Michigan Bariatric Surgery Collaborative, this clinical decision support tool provides risk stratification for bariatric surgery candidates. The system leverages validated prediction models to generate patient-specific outcomes. By processing clinical data such as comorbidities, demographics, and planned procedure type, the interface calculates projected 1-year weight loss, 30-day serious complication risk, and venous thromboembolism (VTE) probability. The VTE module also generates risk-stratified treatment guidelines, facilitating informed preoperative counseling and surgical planning.
Evidence & Research Context
- The core risk prediction models were developed and internally validated using a prospective clinical registry of over 25,000 bariatric surgery patients in Michigan.
- The weight loss calculator was validated in a U.S. Hispanic population (N=276), demonstrating strong agreement between predicted and actual 1-year weight (concordance correlation coefficient = .80).
- An external validation study (N=51,291) in a Dutch population confirmed the serious complication model has good calibration, indicating its generalizability outside the original development cohort.
- A retrospective study (N=1,050) demonstrated the calculator's utility in identifying patients at risk for lower-than-expected weight loss as early as two months post-surgery.
- The venous thromboembolism (VTE) risk model was derived from an analysis of 27,818 patients, identifying significant predictors for risk stratification and prophylaxis guidance.
Intended Use & Scope
This tool is designed for bariatric surgeons and clinicians for preoperative risk assessment and patient counseling. Its primary utility is to facilitate shared decision-making by quantifying individualized outcome probabilities. The calculator provides risk estimates, not diagnostic certainties, and is not a substitute for comprehensive clinical evaluation and professional judgment.
Studies & Publications
Peer-reviewed research associated with this app.
Validation of the Michigan Bariatric Surgery Collaborative outcomes calculator in a Hispanic population
Chaudhry et al. (2025) · Surgery for Obesity and Related Diseases
Accurately predicted weight loss outcomes in Hispanic bariatric surgery patients.
Predicting serious complication risks after bariatric surgery: external validation of the Michigan Bariatric Surgery Collaborative risk prediction model using the Dutch Audit for Treatment of Obesity
Akpinar et al. (2022) · Surgery for Obesity and Related Diseases
Predicted complication risk accurately overall but showed modest ability to distinguish individual risk levels.
App Information
Developer
University of MichiganCategory
Evidence Profile
Validated in clinical trials · Supported by multiple studies
Platforms
Updated
Jan 2026
© 2025 University of Michigan