My Weight Loss Journey
Validated in clinical trials
App Summary
App Screenshots

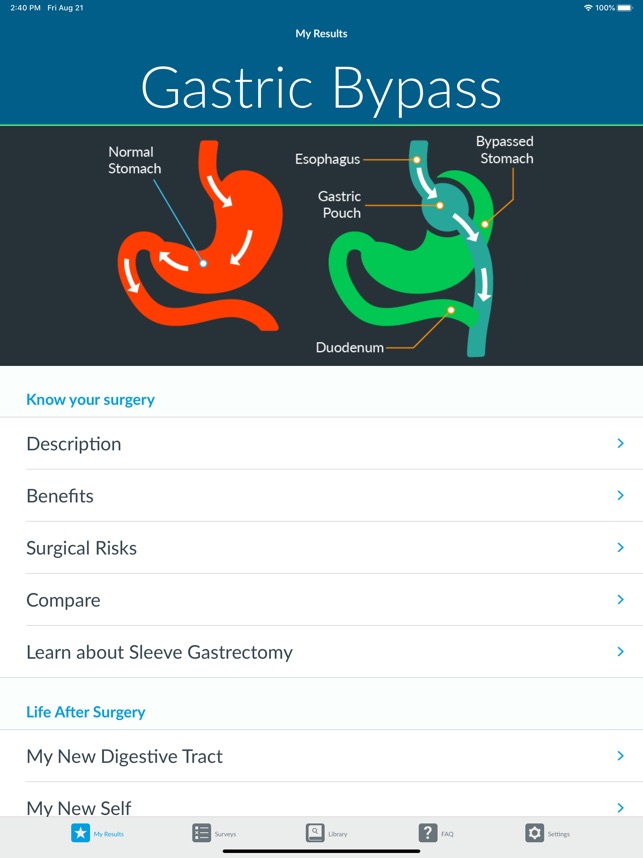
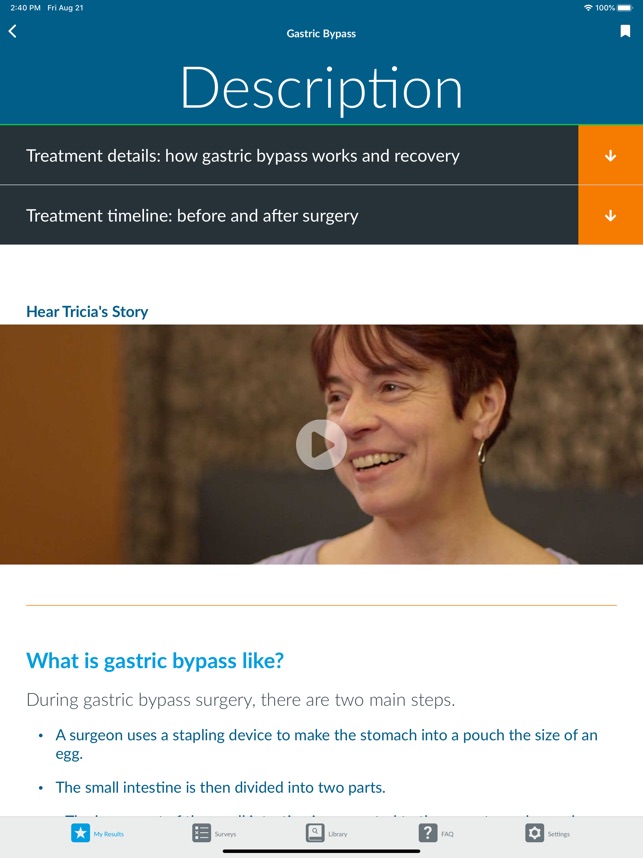





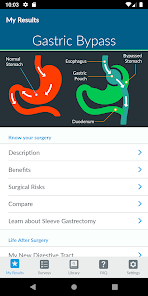
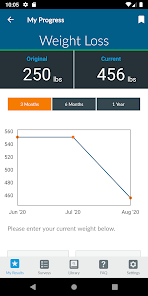

Detailed Description
Functionality & Mechanism
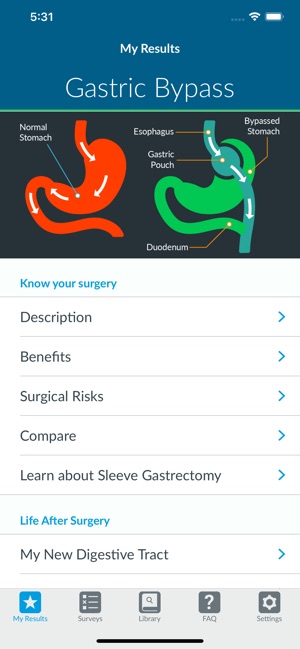
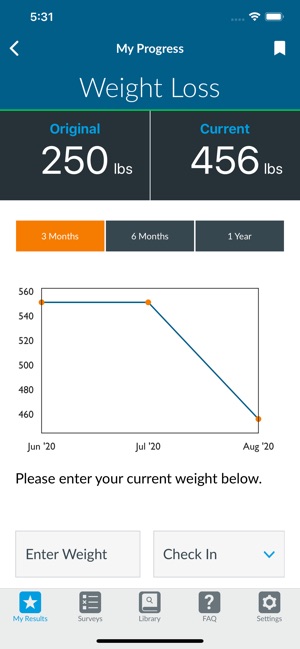
Developed by the University of Michigan and the Michigan Bariatric Surgery Collaborative (MBSC), this application provides tailored risk and benefit estimates for bariatric surgery. The system captures patient data—including demographics, medical history, and procedural preference—via a survey interface. It then generates graphical visualizations of potential outcomes (weight loss, comorbidity resolution) and complications for sleeve gastrectomy and Roux-en-Y gastric bypass. The platform also integrates modules for longitudinal weight tracking and patient engagement through personalized check-ins.
Evidence & Research Context
- The app's proprietary risk/benefit calculator is derived from a prospective, externally-audited clinical registry of over 25,000 patients maintained by the Michigan Bariatric Surgery Collaborative.
- Associated research identified and modeled significant predictors for serious complications (e.g., age, coronary artery disease, mobility limitations) and venous thromboembolism (VTE).
- A validation study (N=276) in a U.S. Hispanic population demonstrated strong agreement between the calculator's predicted weight and patients' actual weight at one year post-surgery (concordance correlation coefficient = .80).
- An external validation study in a Dutch population (N=51,291) confirmed the serious complication model has good calibration, though it showed moderate discrimination (AUC=.602).
Intended Use & Scope
This tool is intended for patients considering bariatric surgery, in collaboration with their clinical care teams. Its primary utility is to facilitate shared decision-making and enhance the informed consent process by providing personalized outcome estimates. The app is not a substitute for clinical consultation and does not provide medical advice or treatment recommendations.
Studies & Publications
Peer-reviewed research associated with this app.
Validation of the Michigan Bariatric Surgery Collaborative outcomes calculator in a Hispanic population
Chaudhry et al. (2025) · Surgery for Obesity and Related Diseases
Calculator accurately predicted weight loss outcomes in Hispanic bariatric surgery patients.
Predicting serious complication risks after bariatric surgery: external validation of the Michigan Bariatric Surgery Collaborative risk prediction model using the Dutch Audit for Treatment of Obesity
Akpinar et al. (2022) · Surgery for Obesity and Related Diseases
Model showed good calibration but only moderate ability to predict serious complication risks.
In the Media
MVC, MBSC Estimate Significant Diabetes Medication Savings Following Bariatric Surgery
The Michigan Value Collaborative (MVC) developed an analysis in partnership with the Michigan Bariatric Surgery Collaborative (MBSC) to assess diabetes medication cost savings following bariatric surgery, using rich administrative claims data sources. The study estimated over $76.5 million in insurance savings on prescription diabetes medications after patients underwent metabolic surgery across Michigan. MVC published their findings in a co-authored research letter in JAMA Surgery, analyzing 760 Type 2 diabetes patients who underwent bariatric surgery between 2015 and 2021.
Bariatric Surgery Risk Scoring Tool May Predict Serious Complications
Dr. Jonathan F. Finks from the University of Michigan developed a population-based risk scoring system to help surgeons predict serious complications following bariatric surgery and select the best procedure for patients, using data from Michigan's comprehensive statewide registry. The tool analyzed 25,469 primary bariatric surgeries performed from June 2006 through December 2010, revealing a 30-day serious complication rate of 2.5% with a 0.1% mortality rate. The research was presented at the annual meeting of the American Surgical Association in Boca Raton, Florida.
App Information
Developer
University of MichiganCategory
Evidence Profile
Validated in clinical trials
Platforms
Updated
Sep 2025
© 2025 University of Michigan