NIH Stroke Scale Calculator
Validated in clinical trials
App Summary
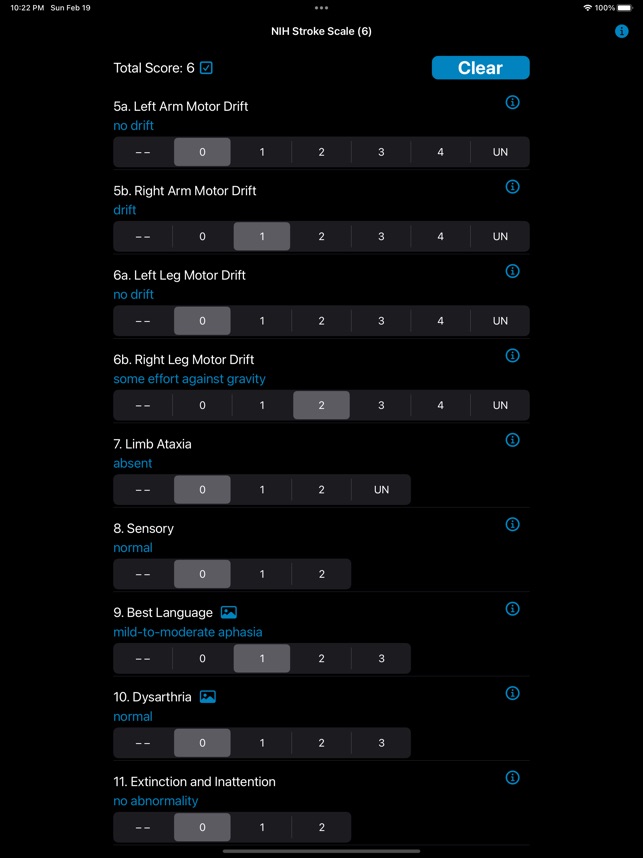
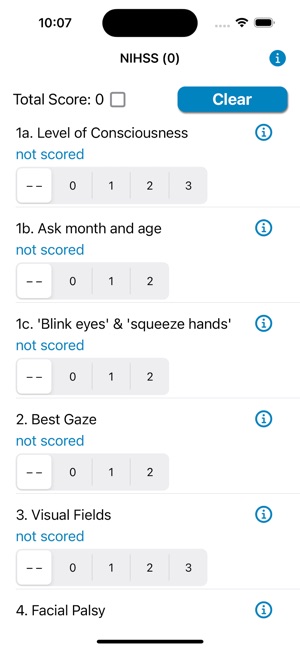
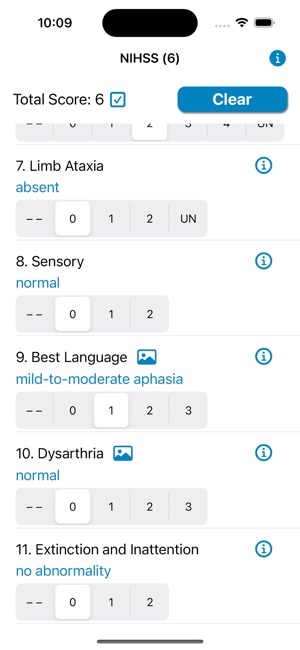
App Screenshots


Detailed Description
Functionality & Mechanism
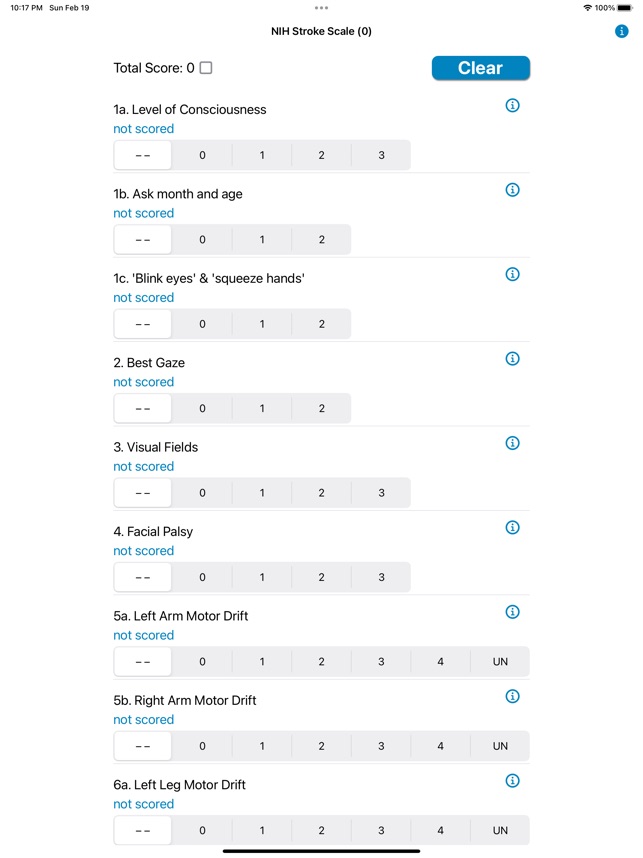
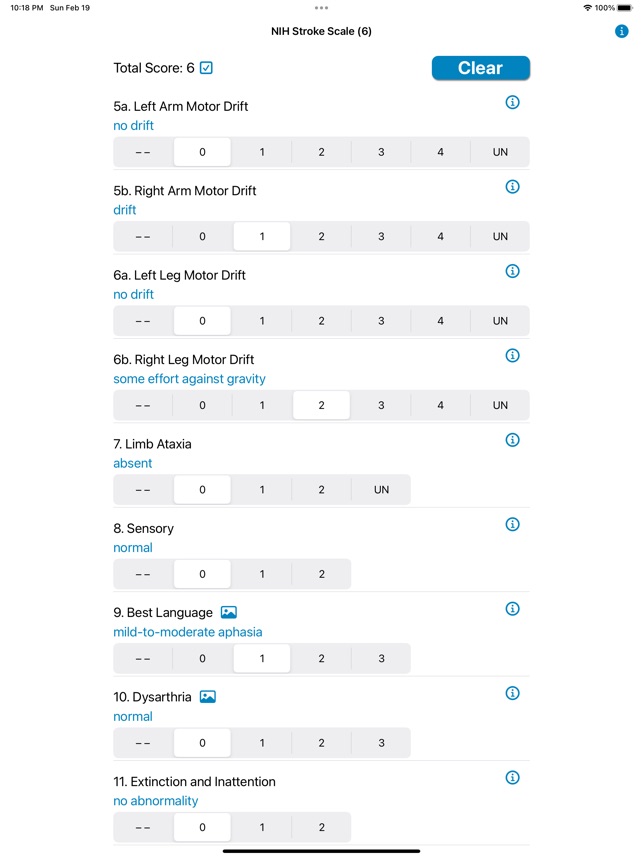
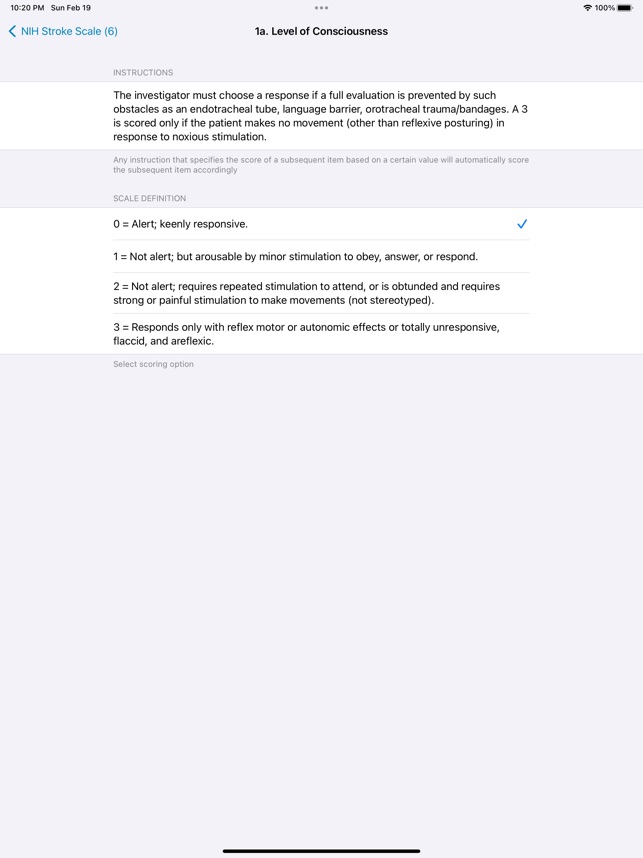
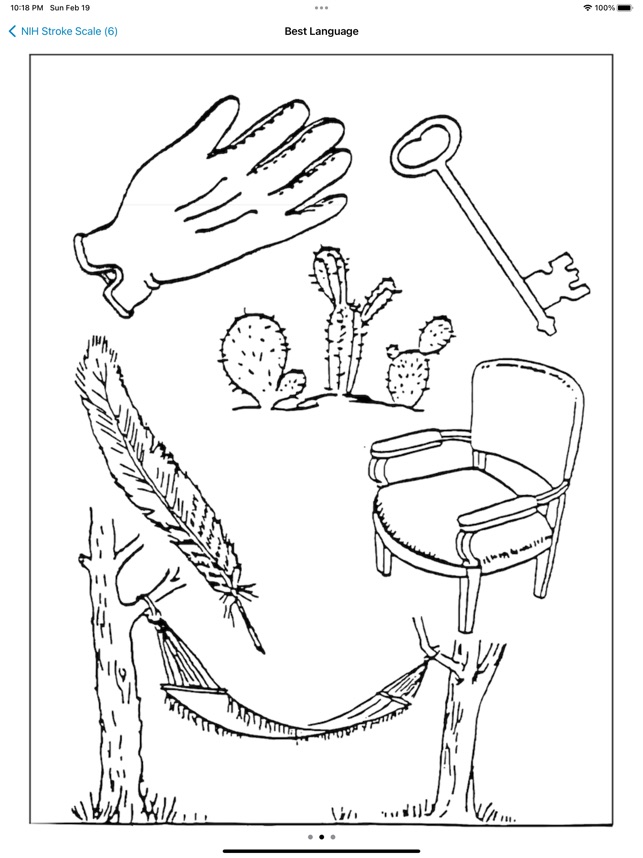
The NIH Stroke Scale Calculator digitizes the standardized 15-item neurologic examination for acute stroke assessment. The interface systematically guides clinicians through each component of the scale, from level of consciousness to limb ataxia and sensory loss. Input is captured via responsive controls, facilitating a more rapid evaluation compared to manual methods. The system then automatically computes a final score to quantify the severity of the neurological deficit, streamlining a critical component of the acute stroke workflow.
Evidence & Research Context
- The underlying NIH Stroke Scale demonstrates robust inter- and intra-rater reliability (intraclass correlation coefficients >.93) across various rater roles, including neurologists, emergency physicians, and nurses.
- In foundational validation research (N=65), prospective NIHSS scores correlated strongly with both CT-measured infarction size (r=0.68) and 3-month clinical outcomes (r=0.79), supporting the scale's predictive validity.
- The scale's reliability has been explicitly extended to non-neurologist physicians and non-physician study coordinators, confirming its utility for multidisciplinary stroke teams with standardized training.
Intended Use & Scope
Designed for clinicians, including physicians and nurses, as a point-of-care tool for the rapid assessment of patients with suspected ischemic stroke. The calculator facilitates standardized scoring to quantify neurological deficits. It is not a standalone diagnostic instrument and does not replace clinical judgment; all outputs require interpretation by a qualified professional.
Studies & Publications
Peer-reviewed research associated with this app.
Reliability of the National Institutes of Health Stroke Scale. Extension to non-neurologists in the context of a clinical trial
Goldstein et al. (1997) · Stroke
Non-neurologists can reliably use the NIHSS stroke scale with the same accuracy as neurologists.
Measurements of acute cerebral infarction: a clinical examination scale
Brott et al. (1989) · Stroke
Stroke scale reliably measures stroke severity and accurately predicts lesion size and patient outcomes.
App Information
Developer
US Department of Veterans AffairsCategory
Evidence Profile
Validated in clinical trials
Platforms
Updated
Jun 2023
© 2025 US Department of Veterans Affairs
Tags
Developer Links
Privacy PolicyNIH Stroke Scale Calculator
Free