OHSU MViPS
Proven effective in research studies · Supported by multiple studies
App Summary
App Screenshots
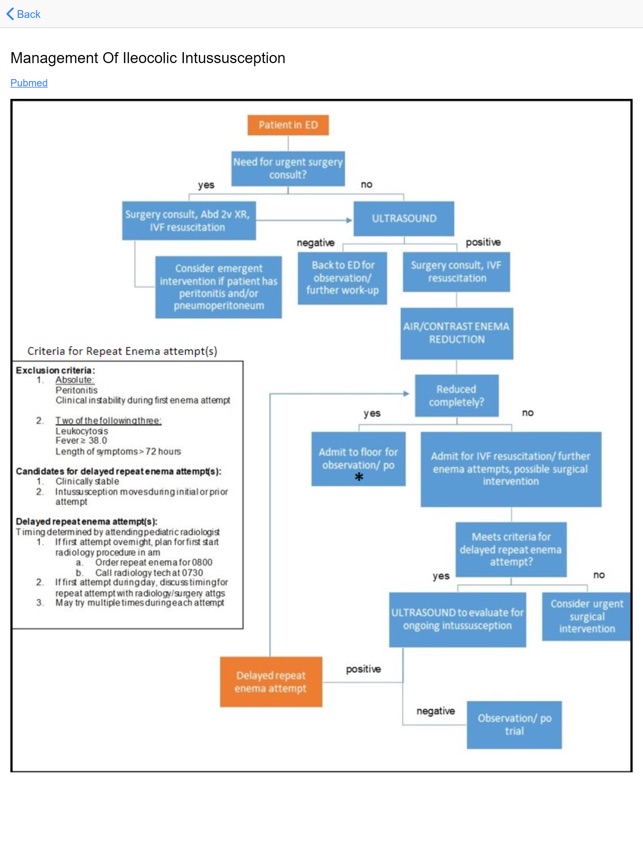


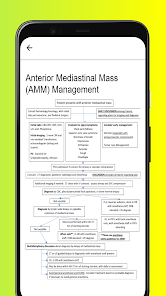
Detailed Description
Functionality & Mechanism
Developed by Oregon Health & Science University, OHSU MViPS is a clinical reference system that provides access to standardized protocols from the Minimizing Variance in Pediatric Surgery program. The interface facilitates retrieval of evidence-based perioperative pathways for a range of pediatric surgical conditions. By centralizing these guidelines, the system is designed to reduce practice variation and promote consistent, high-quality care. It also provides direct links to the supporting published research for each protocol.
Evidence & Research Context
- A multi-institution cohort study (N=1081) evaluating the MViPS program found that protocol implementation was associated with a 23% shorter length of stay and a 10% reduction in total hospital costs, with no change in complication rates.
- A retrospective study (N=145) on a perioperative colon bundle demonstrated a significant decrease in superficial surgical site infections (21% to 8%) and readmissions (16% to 4%) post-implementation.
- In a two-center study (N=106) of a protocol for pediatric blunt solid organ injury, significant reductions were observed in hospital stay (4.6 vs. 3.5 days) and ICU stay (1.9 vs. 1.0 days).
- Implementation of a standardized gastrostomy protocol (N=65) was associated with a shorter length of stay while maintaining similar patient complication rates across treatment groups.
Intended Use & Scope
The OHSU MViPS system is intended for pediatric surgeons, trainees, and affiliated clinicians as a point-of-care reference tool for practice standardization. Its primary utility is to facilitate the adoption of evidence-based perioperative protocols. This tool does not supplant clinical judgment, which is required to appropriately apply protocols to individual patient cases.
Studies & Publications
Peer-reviewed research associated with this app.
Standardized Perioperative Protocols and Variance in Pediatric Surgery
Selesner et al. (2025) · JAMA Surgery
Achieved 23% shorter hospital stays with similar complication rates across multiple procedures.
Minimizing variance in pediatric surgical care through implementation of a perioperative colon bundle: A multi-institution retrospective cohort study
Cunningham et al. (2020) · Journal of Pediatric Surgery
Reduced surgical site infections and readmissions after colorectal procedures.
App Information
Developer
Oregon Health & Science UniversityCategory
Evidence Profile
Proven effective in research studies · Supported by multiple studies
Platforms
Updated
Feb 2026
© 2025 Oregon Health & Science University