UB-CAM Delirium Screen
Proven effective in research studies
App Summary
App Screenshots
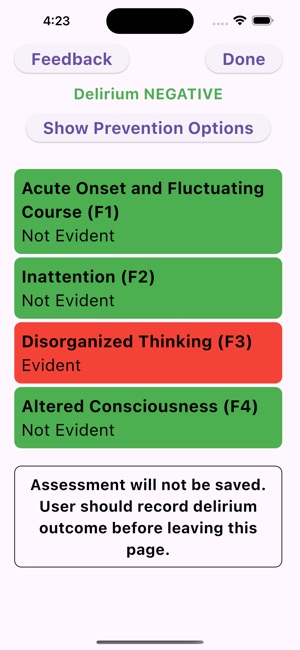
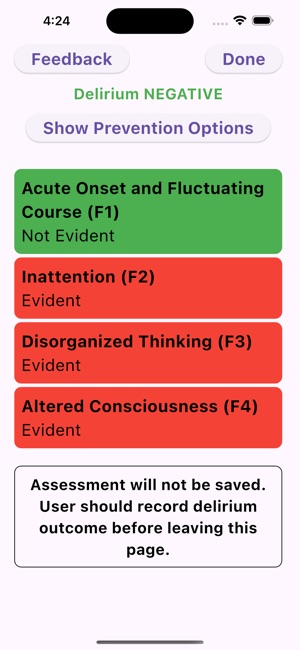
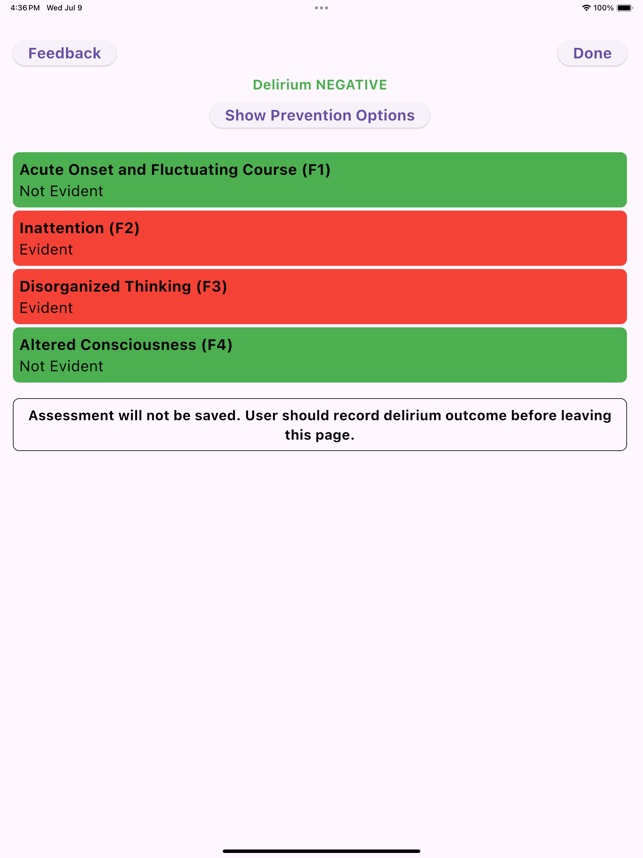

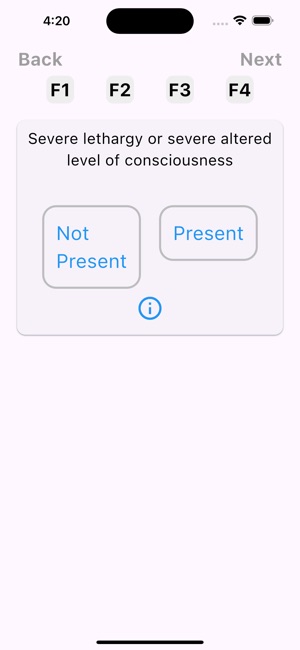
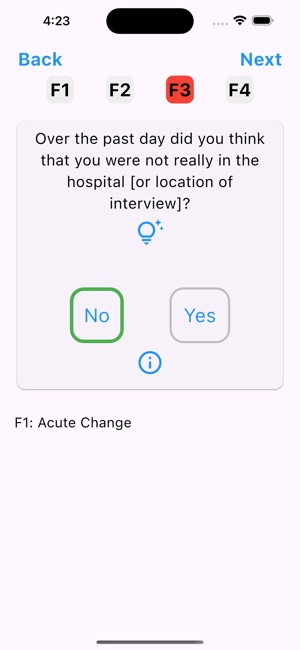





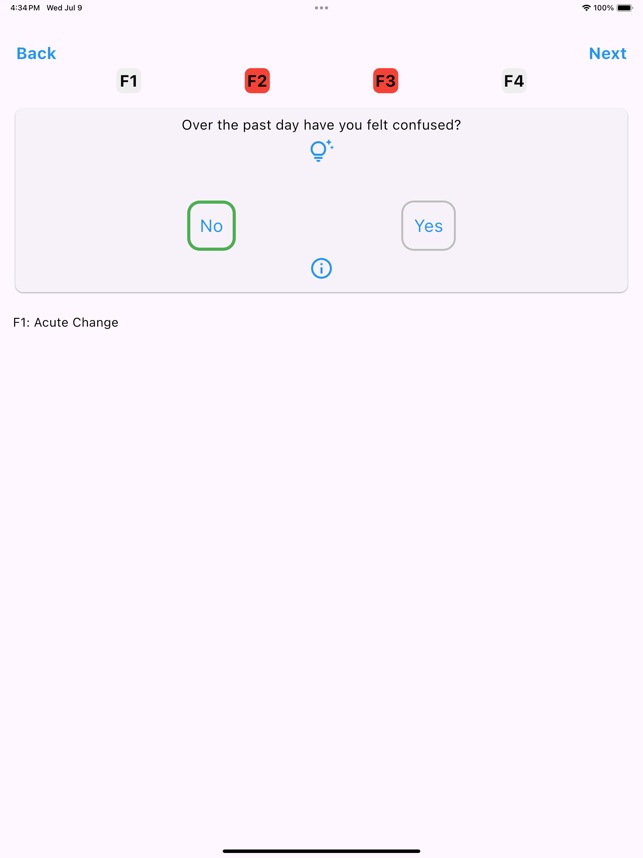




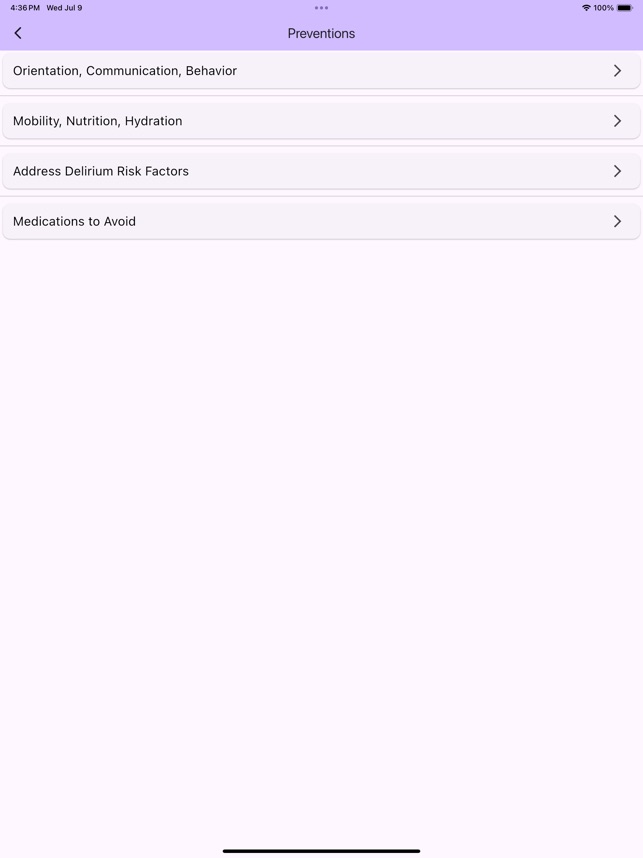






Detailed Description
Functionality & Mechanism
The UB-CAM Delirium Screen operationalizes a two-step protocol for identifying delirium in hospitalized adults. Developed by a clinical research team, the app first administers the 2-item UB-2 screen. If results indicate potential delirium, the interface automatically proceeds to the 3D-CAM diagnostic assessment. The entire app-directed protocol requires approximately 90-110 seconds to complete. The system stores prior assessments to facilitate automatic detection of acute mental status changes and integrates with REDCap for data management.
Evidence & Research Context
- A prospective diagnostic study (N=527 hospitalized older adults) validated the two-step protocol, demonstrating specificities of 93% (nurses) and 91% (physicians), with sensitivities of 65% and 63% respectively.
- The app-directed protocol is efficient, requiring an average administration time of 90 to 110 seconds across studies involving physicians, nurses, and research assistants.
- A preliminary pilot study (N=11) in older adults with mild dementia indicated robust inter-rater reliability, with 100% agreement on delirium status in paired assessments.
- Implementation evaluations report high feasibility, with clinician protocol completion rates exceeding 97% and strong qualitative feedback on usability from diverse clinical users.
Intended Use & Scope
This tool is designed for clinicians, including physicians, nurses, and nursing assistants, to conduct rapid, systematic bedside screening for delirium in hospitalized adults. Its primary utility is the early identification of potential delirium cases that warrant further investigation. The app does not provide a medical diagnosis; a positive screen necessitates a comprehensive clinical evaluation.
Studies & Publications
Peer-reviewed research associated with this app.
A Pilot Study Testing the iOS UB-CAM Delirium App
Kuzmik et al. (2023) · Journal of the American Geriatrics Society
Successfully developed iOS app with improved accessibility, clear instructions, and clinical result-saving features.
Comparative Implementation of a Brief App-directed Delirium Identification Protocol by Hospitalists, Nurses, and Nursing Assistants
Marcantonio et al. (2022) · Annals of Internal Medicine
App-directed delirium screening was feasible and accurate across all clinician types with 97% completion rates.
In the Media
$3.8M grant to boost delirium screening, improve older adult safety
Penn State researchers secured a $3.8 million grant from the National Institutes of Health's National Institute on Aging to address delirium in hospitalized older adults, as more than half of all cases go undetected in routine care. Delirium, a sudden and usually reversible confusion, often leads to physical and cognitive decline, nursing home placement, and even death with devastating outcomes for individuals and care partners. The interdisciplinary team of researchers and community partners will work to improve delirium screening and older adult safety.
Two-step screening app supports quick identification of delirium
Penn State's Ross and Carol Nese College of Nursing developed a two-step screening app based on the Ultra-Brief 2-Item Screener (UB-2) and 3-minute Diagnostic Confusion Assessment Method (3D-CAM) to enable quick delirium detection and treatment. In step one, clinicians use the UB-2 to ask patients two questions determining if the 3D-CAM assessment is warranted in step two. Moving these tools to an app-delivered format makes usage easier and enables faster identification of delirium in hospitalized older adults.
Nursing faculty and team identify time-efficient, delirium-screening protocol
Harvard University's Edward Marcantonio partnered with Penn State College of Nursing professors Donna Fick, Marie Boltz, and Project Director Erica Husser to examine four delirium identification assessment protocols for improving time efficiency and delirium identification. The research team studied 201 inpatients aged 75 years or older at an urban academic medical center to better understand how to combat the significant problem of undetected delirium in hospitalized older adults. The collaborative study aimed to develop more efficient screening methods.
App Information
Developer
Pennsylvania State UniversityCategory
Evidence Profile
Proven effective in research studies
Platforms
Updated
Nov 2025
© 2025 Pennsylvania State University