MOVE! Coach
Studied in clinical trials · Mixed evidence
App Summary
App Screenshots





Detailed Description
Functionality & Mechanism
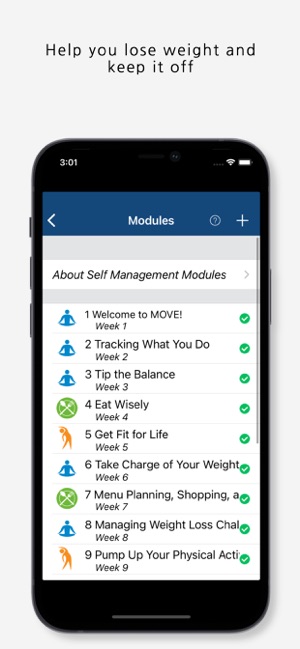
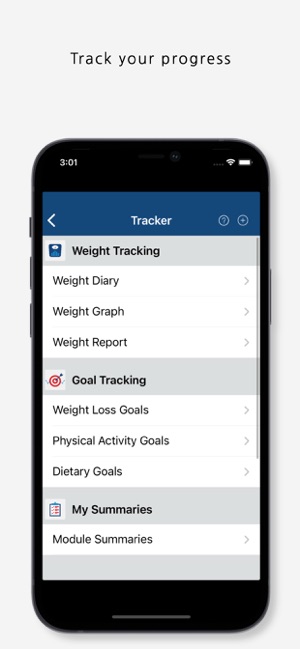
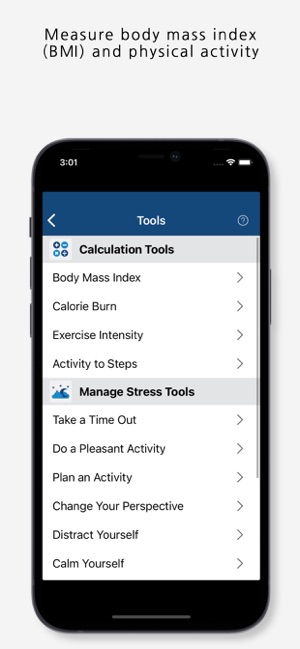
Developed by the VHA's National Center for Health Promotion and Disease Prevention, MOVE! Coach delivers a structured 16-week weight management program. The system provides users with sequentially unlocked weekly modules containing pedagogical content via videos, worksheets, and interactive tools. Core functionality includes self-management modules, goal-setting interfaces, and progress trackers for weight, diet, and exercise. The app can be used as a standalone intervention or in conjunction with clinical care and integrates with Apple HealthKit for data synchronization.
Evidence & Research Context
The following evidence pertains to the multicomponent MOVE! program, which provides the clinical framework for the app:
- An effectiveness study (N=377) found that veteran participants achieved an average weight loss of 2.2 kg at one year post-enrollment, reversing a pre-enrollment trend of weight gain.
- Program evaluation data indicates a dose-response relationship, where more intensive participation (≥6 encounters) was associated with significantly greater weight loss (−3.7 lbs) at 12-month follow-up compared to nonparticipants.
- A preliminary pilot study (N=14) of veterans with severe obesity and depression found program participation was associated with significant reductions in depression severity, which correlated with weight loss.
- A randomized trial (N=109) of a modified program for veterans with serious mental illness did not demonstrate a significant effect on weight loss, indicating variable outcomes across specific clinical populations.
Intended Use & Scope
This app is intended for use by veterans, service members, and the general public as a self-guided weight management tool. Its primary utility is to deliver a structured behavioral intervention and facilitate progress monitoring. The app does not replace professional medical advice or treatment for obesity-related comorbidities and should be used in consultation with a healthcare provider, particularly for individuals with complex medical histories.
Studies & Publications
Peer-reviewed research associated with this app.
National Veterans Health Administration MOVE! Weight Management Program Participation During the COVID-19 Pandemic
Gray et al. (2022) · Preventing Chronic Disease
The weight management program successfully transitioned to virtual care during COVID-19 with sustained participation levels.Antidepressant Effect of the VA Weight Management Program (MOVE) Among Veterans With Severe Obesity
Shiroma et al. (2020) · Military Medicine
Showed trends toward depression improvement but lacked statistical significance and a comparison group.
In the Media
MOVE! Coach
The U.S. Department of Veterans Affairs developed MOVE! Coach to help Veterans, service members, and their families manage their weight using convenient mobile education and resources. The app provides users with self-management modules, progress tracking tools, and goal-setting features that allow them to "monitor their progress with their health and weight goals." Users can create personal health and physical activity goals while sharing them via social media for additional support.
VA News and Information
The Department of Veterans Affairs developed MOVE! Coach to help veterans manage weight and improve fitness through a mobile platform integrated with VA health services. The app requires users to enter the same login credentials they use for VA.gov for security purposes and puts VA health and benefit information at users' fingertips anywhere, anytime. The application is available through VA's mobile health platform alongside other veteran-focused digital health tools.
Get moving with the MOVE! Coach app
The VA developed MOVE! Coach to provide Veterans and others with a 16-week weight management and lifestyle program using behavioral strategies and educational support. "What sets MOVE! Coach apart from other diet and activity apps is the strong educational support," said Lori Carlson, registered dietitian nutritionist and MOVE! program analyst. Retired Air Force Veteran Christy Blaum successfully lost 34 pounds using the app and continues using it for daily accountability.
MOVE! Coach
The Department of Veterans Affairs developed MOVE! Coach to support weight management for Veterans, using a self-management tool with educational content and progress tracking that can be used independently or with VA facility team check-ins. The app features 16 weekly self-management modules where "each module has an overview, educational content, videos and activities and an opportunity to set goals." While designed for Veterans, the app is available for anyone to use, though only Veterans can access check-ins with VA facility MOVE! teams.
Mobile app helps Veteran drop weight and live healthily
The VA developed MOVE! Coach to help Veterans manage weight loss through a 19-week self-guided program that tracks diet, physical activity and weight goals. Navy Veteran Richard Dalton used the app to drop more than 60 pounds over several months, stating "Through MOVE! Coach I have gotten my blood sugar down to normal." Dalton credits the app's convenience, noting "My smartphone is always with me, making it easy to use MOVE! Coach to write down what I'm eating, while I'm eating."
App Information
Developer
US Department of Veterans AffairsCategory
Evidence Profile
Studied in clinical trials · Mixed evidence
Platforms
Updated
Apr 2026
© 2025 US Department of Veterans Affairs